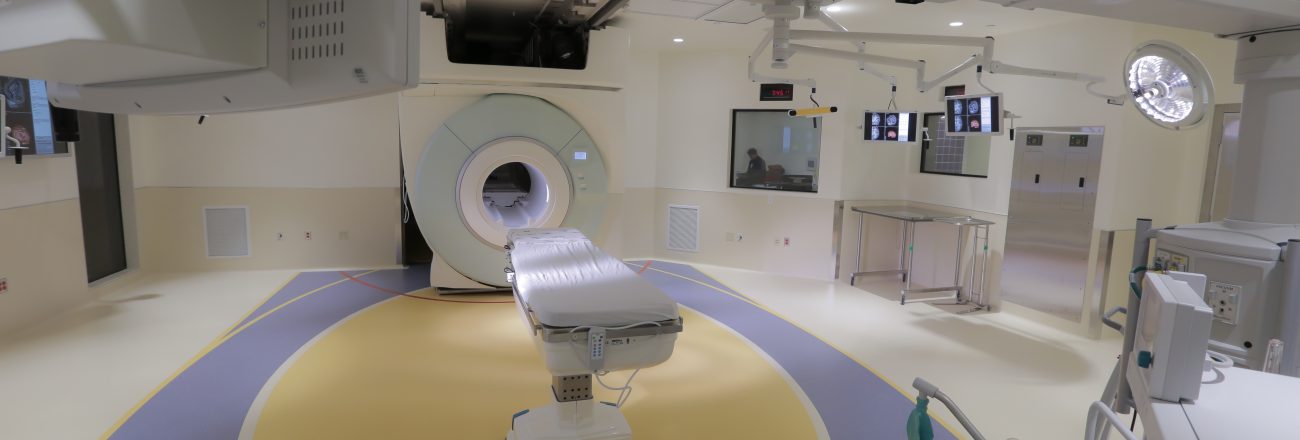
First Intraoperative MRI (iMRI) Equipment on the West Coast
“This machine is a total game changer, “ according to Dr. Nathan Selden, Chair of Department of Neurological Surgery. “ It’s particularly unusual in a children’s hospital, and it will have a very high impact for OHSU adult and pediatric patients.”
Oregon Health & Sciences University (OHSU) Doernbecher is the first dedicated children’s hospital on the West Coast to open a pediatric iMRI (intraoperative magnetic resonance imaging) facility within the hospital’s operating room.
Life prior to iMRI status.
Consider a typical operating room, with just enough space for the clinicians, bed + patient and essential tools to get the job done. Generally the clinicians have a “road map” (i.e. including the MRI scan) for how the procedure will be executed. Now consider a brain operation… You don’t have to have an M.D. behind your name to infer that this may be somewhat more complicated, procedurally. Given the intricacies of this vital organ, the first “road map” may not be sufficient. Often, a second (or even third) MRI scan is needed during an operation, to confirm a step in the procedure. To start and stop and start again, since we’re talking about the BRAIN—master circuit board of the body—this might be the epitome of invasiveness. Imagine the trauma inflicted on a adult, much less a child, undergoing multiple brain surgeries. But what if the MRI equipment could be accessible IN the operating room DURING the operation??
The answer is, it can. It’s called an Intraoperative MRI (iMRI).
The magic behind the scenes.
In 2013, Mazzetti became the MEP Lead to make this very challenging expansion a reality for OHSU’s Doernbecher Children’s Hospital, working alongside the Architect SRG Partnership, General Contractor Hoffman Construction, Structural Engineer KPFF, and Landscape Architect & Civil Engineer WH Pacific.
The expansion was carved into a hillside inflicting physical constraints coupled with the existing infrastructure constraints.
New equipment was installed including a new surgery air handler, which now back-feeds the existing surgery suite, in addition to an emergency exhaust system and an oxygen monitoring system to maintain safety in the IMRI suites. Numerous modifications to existing electrical and hydronic infrastructure were employed to support this new imaging suite. Extensive BIM coordination was executed to facilitate integration of the many different services.
The first performance received RAVING reviews.
Check out an excerpt from Dr. Nate Selden’s email (to the project team) shortly after the first procedure, completed in March…
The operation, for medically refractory epilepsy, went beautifully. Images obtained after the initial resection showed a small amount of residual lesion adjacent to critical eloquent cortex. The new images were instantaneously networked to the operative navigation computer, the residual was safely removed, and the final result was confirmed by a second intra-operative scan; no inpatient scans are now required post-operatively. The clinical outcome today is marvelous, and likely to be transformative for this child both in terms of disease resolution and maintenance of vital neurological function.
I am confident in this case we avoided not only a second separate craniotomy, but also two associated post-operative (sedated) scans.
Hear more from Dr. Selden in this short video: